Medical Dermatology
Basal Cell Carcinoma in Dallas
- Home
- Medical Dermatology
- Skin Cancer
- Basal Cell Carcinoma in Dallas
Find Treatment for the Most Common Form of Skin Cancer
Dr. Ellen Turner can successfully treat your biopsy-proven basal cell carcinoma at her Dallas-based practice. Basal cell carcinoma, deriving itself from the bottom-most or basal layer of the skin, is the most common type of cancer, as well as the most common type of skin cancer.
Medical Dermatology
Contact us online about setting up an appointment or call (214) 373-7546. Find out more about what to do about basal cell carcinoma in the Dallas area today.
How Do I Know if I Have Basal Cell Carcinoma?
Diagnosis of basal cell carcinoma requires a biopsy, or a sample of the skin cells. To do this, Dr. Turner and her trained staff will locally anesthetize the area to be sampled and take a surgical blade to remove the needed cells. The skin specimen will be sent to a pathology lab for review by a certified dermatopathologist, someone who is trained specifically in conditions related to the skin only. If there appears to be malignant cells, the dermatopathologist will note how deep the cells penetrate. If the cells remain high in the layers of skin, the cancer may be considered superficial. In the case where all of the layers of skin are affected, it is considered to be nodular. The depth of penetration and the amount of invasion of the basal cell carcinoma will determine the proper treatment options Dr. Ellen Turner can recommend for the patient.
What Does a Basal Cell Carcinoma Look Like?
Basal cell carcinoma can appear in various forms—some appear to be more pearly in coloration with evidence of fine blood vessels, or telangiectasias running throughout the abnormal tissue. Other basal cell carcinomas, also commonly abbreviated as BCC, can be shiny pink and scaly when superficial or even pigmented in coloration, depending on the background skin color of the individual.
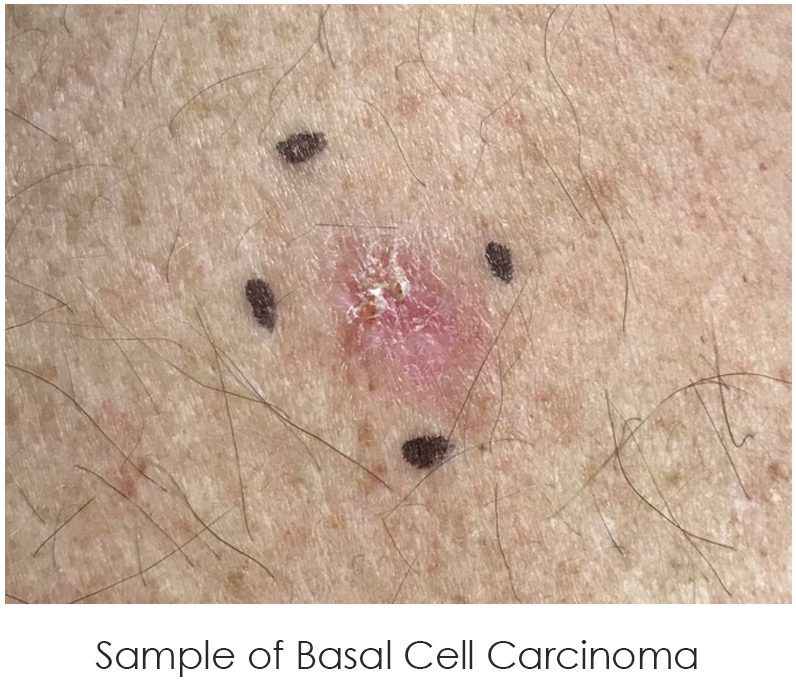
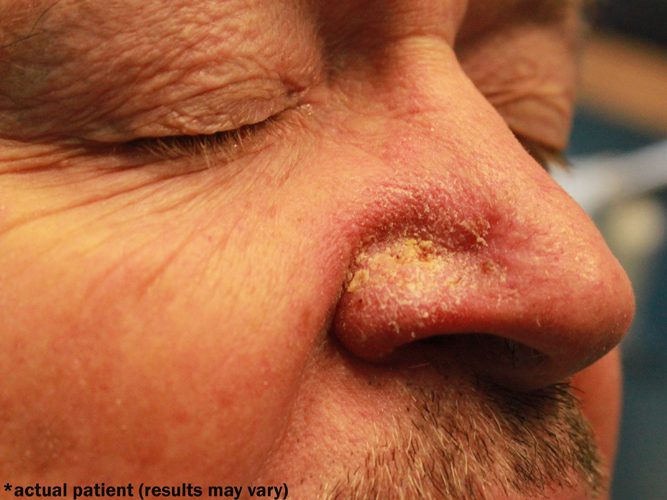
*Patient results may vary
Will a Basal Cell Carcinoma Spread Internally and Hurt Me?
Basal cell carcinoma grows so slowly over time, it can sometimes be easy for patients to ignore the warning signs: new lesion, growing lesion, or changes in the appearance of a lesion. However, many basal cells can break the skin down and lead to bleeding, which oftentimes prompts patients to come to the dermatologist, such as Dr. Ellen Turner, for diagnosis and treatment.
Basal cell carcinoma, when caught early, can be easily treated. Even if basal cell carcinomas are allowed to slowly grow over many months, and even years, treatment is still very possible and can allow for a normal life span and good quality of life. However, it is always best to diagnose basal cell carcinoma as early as possible in order to minimize the amount of treatment required to ensure the cancer has been successfully and completely treated.
How is Basal Cell Carcinoma Treated?
Fortunately, there are multiple ways to appropriately and adequately treat basal cell carcinoma/cancer. These can include surgical excision by the dermatologist who performed the initial biopsy, or by a specialized Mohs surgeon. Mohs surgery requires specific criteria that a trained dermatologist, such as Dr. Ellen Turner, will know. She can properly direct and guide patients if that is the best treatment option for that particular basal cell carcinoma based on location such as a nose, ear, or eyelid where there is not a lot of excess tissue that can be removed indiscriminately.
Whether excisional surgery or Mohs surgery is opted for by the basal cell carcinoma patient, it typically requires a few hours to perform the procedure, while the patient is awake and ambulatory. There is no need, typically, for patients to ever be hospitalized or even admitted to outpatient surgery centers for the surgical excision of the cancer. The area is locally anesthetized, and the excision is performed. If there is a regular excision being performed, the American Academy of Dermatology recommends the surgeon include a 4mm margin on all sides surrounding the visualized abnormal cells to ensure the best possible cure rate so that even non-visual cells will be completely removed. The final result of a surgery is always a scar. Scars remodel themselves and continue to improve in appearance for a period of four to six months post-procedure.

When Mohs surgery is performed, the patient is still locally anesthetized, and the first layer is removed and examined microscopically while the wound is still open. If there are remaining cells visualized, the surgeon repeats another removal or “layer” until which time there are no cells visualized. This allows no additional margin taken, but assurance that the malignancy is completely gone. As with traditional excision, Mohs surgery leaves a scar.
When basal cell carcinomas are still diagnosed at biopsy as being superficial, or as only existing in the topmost layers of the skin, possible treatment options include topical therapy such as imiquimod, which is an immunomodulator cream that can be applied to the skin surface for a period of a few weeks. When this imiquimod is used, the area being treated reacts with redness, swelling, and crusting, which is considered normal. Many times, the border around the actual treatment area reacts as well in the same fashion, and this is called a “field effect.” In the case of the field effect, even cells that are not visualized with the naked eye are being cleaned up by the imiquimod due to detection of abnormal cellular change consistent with pre-cancer and cancer.
Additional treatment for superficial basal cell carcinoma is electrodessication and curettage of the area. A curette tool is a surgical instrument used to scrape the layers of skin off, and a hyfrecator or electric current is used to stop the pinpoint bleeding and create additional destruction of the cells. The procedure, commonly abbreviated as ED&C, is repeated for a total of three times to ensure clearance of the abnormal cells. Healing from ED&C is slower than traditional excision or Mohs surgery as the cells must heal secondarily as opposed to primarily, but the final scar results are good when these procedures are performed on proper body location sites.

A more recent and very exciting development in the treatment options for basal cell carcinoma is the use of superficial radiation specifically designed to treat skin malignancies such as basal cell carcinoma and squamous cell carcinoma. This non-scarring, painless treatment allows for an appropriate amount of radiation to be targeted into the focus of abnormal cells to include a margin in order to give the same cure rate as Mohs surgery. In particularly sensitive cosmetic areas such as the nose, ear, or eyelid, or even in areas such as the front of the lower leg, radiation provides an excellent final result minus the scarring. Many patients are opting for this therapy, and Dr. Ellen Turner’s patients are fortunate to have access to this newer technology in the Dallas/Fort Worth area.
Regardless of how a patient and Dr. Ellen Turner elect to treat a basal cell carcinoma, it is important to continue to monitor a skin cancer patient by performing a simple and painless full body skin exam twice yearly, or every six months in order to catch any new or changing lesions early and get the best possible outcome.

