Medical Dermatology
Psoriasis
- Home
- General Dermatology
- Psoriasis
Psoriasis Description, Diagnosis and Treatment
What is psoriasis and how is it diagnosed in the Dallas area?
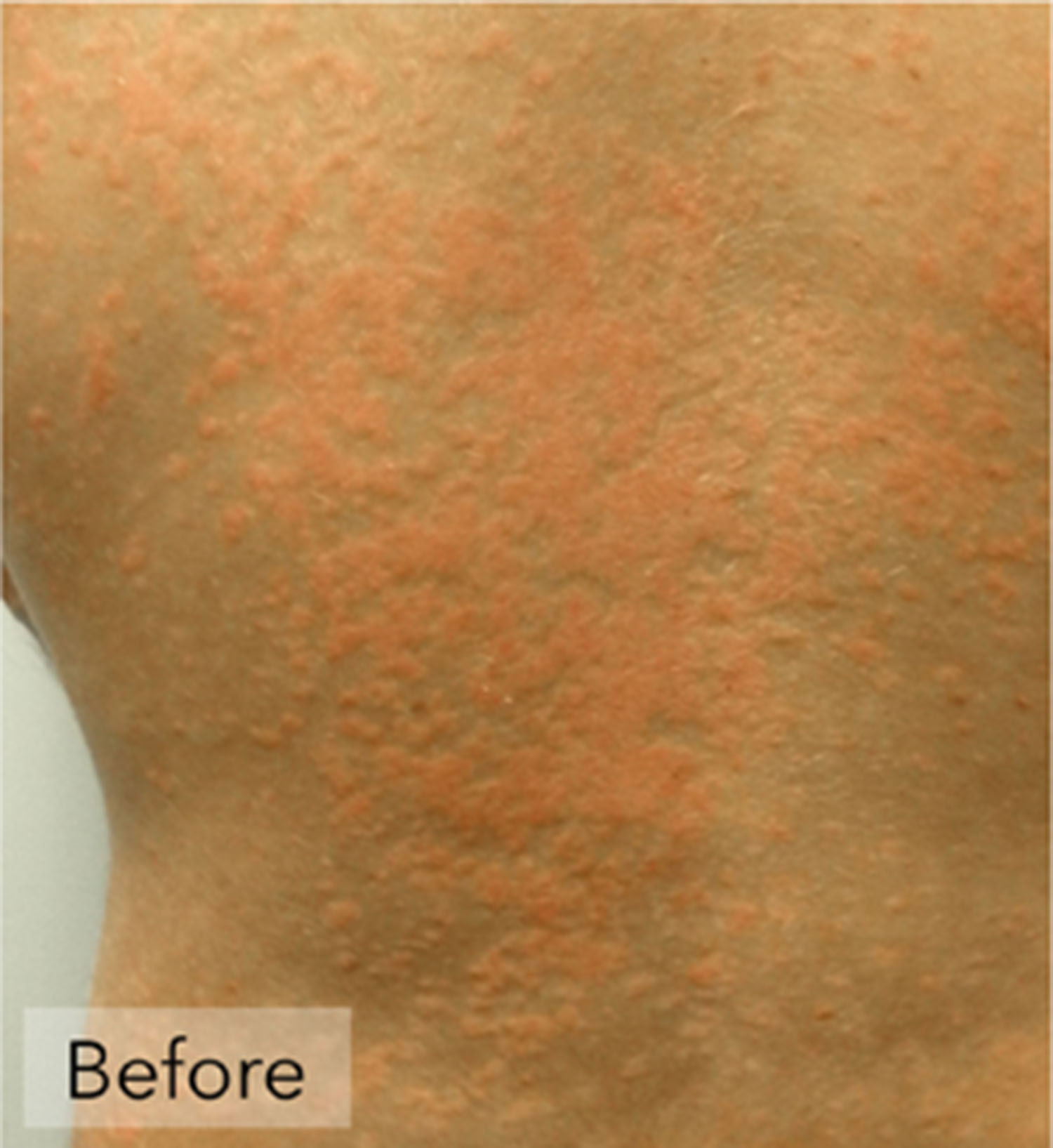
 Psoriasis is a persistent skin disorder in which there are red, thickened areas with silvery scales, most often on the scalp, elbows, knees and lower back. Some cases of psoriasis are so mild that people don’t know they have it. Severe psoriasis may cover large areas of the body. Dermatologists are the primary specialty to help even the most severe cases.
Psoriasis is a persistent skin disorder in which there are red, thickened areas with silvery scales, most often on the scalp, elbows, knees and lower back. Some cases of psoriasis are so mild that people don’t know they have it. Severe psoriasis may cover large areas of the body. Dermatologists are the primary specialty to help even the most severe cases.
Psoriasis is not contagious and cannot be passed from one person to another, but it is most likely to occur in members of the same family. In the United States, two out of every hundred people have psoriasis (four to five million people). Dermatologists diagnose psoriasis by examining the skin, nails and scalp. If the diagnosis is in doubt, a skin biopsy may be helpful.
Medical Dermatology
Book an appointment online or call (214) 373-7546 to schedule an appointment to see us in our Dallas or Irving locations.
What causes psoriasis?
The cause is unknown. However, recent discoveries point to an abnormality in the functioning of special white cells (T-cells) that trigger inflammation and the immune response in the skin. Because of the inflammation, the skin grows too rapidly. Normally, the skin replaces itself in about 30 days, but in psoriasis, the process speeds up and replaces the skin in three to four days, and the signs of the disorder develop.
People often notice new spots 10 to 14 days after the skin is cut, scratched, rubbed or severely sunburned (Koebner Phenomenon). Psoriasis can also be activated by infections, such as strep throat, and by certain medicines (beta blockers, lithium, etc.). Flare-ups sometimes occur in the winter, as a result of dry skin and lack of sunlight.
What are the types psoriasis?
Psoriasis comes in many forms. Each differs in severity, duration, location, shape and pattern of the scales. The most common, called plaque psoriasis, begins with little red bumps. Gradually, these become larger, and scales form. While the top scales flake off easily and often, scales below the surface stick together. These small red areas can enlarge.
-
- Scalp, elbows, knees, legs, arms, genitals, nails, palms and soles are the areas most commonly affected by psoriasis. It will be often appear in the same place on both sides of the body.
- Scalp psoriasis may be mistaken for dandruff.
- Nails with psoriasis frequently have tiny pits in them. Nails may loosen, thicken or crumble, and are difficult to treat.
- Inverse psoriasis occurs in the armpit, under the breasts and in skin folds around the groin, buttocks and genitals.
- Guttate psoriasis usually affects children and young adults. It often starts after a sore throat with many small, red, scaly spots appearing on the skin. It frequently clears up by itself in weeks or a few months.
- Up to 30 percent of people with psoriasis may have symptoms of arthritis, and 5 to 10 percent may have some functional disability from arthritis of various joints. In some people, the arthritis is worse when the skin is very involved. Sometimes the arthritis improves when the condition of the patient’s skin improves.
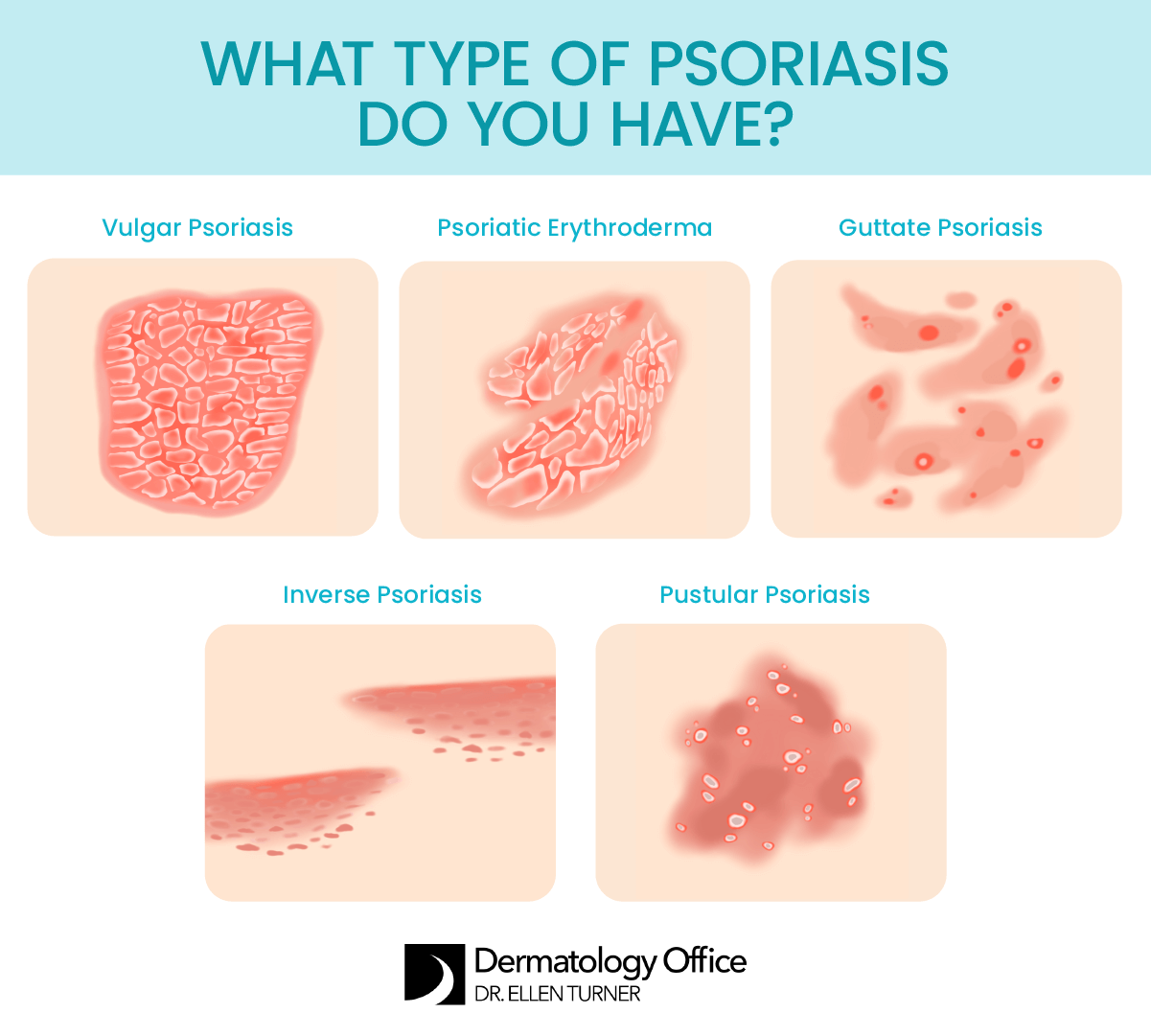
Get diagnosis and treatment for symptoms of psoriasis at the Dallas and Irving-based Dermatology Office of Dr. Ellen Turner. Psoriasis vulgaris is the most common type, typically causing thick and scaly plaques to develop as the skin cell turnover process speeds up. Other variations include guttate (characterized by drop-shaped spots on the limbs and trunk, most often on young people) and inverse (developing as red, inflamed areas in folds on the body), as well as the rare, blistering pustular form and psoriatic erythroferma, which causes body-wide burning rashes.
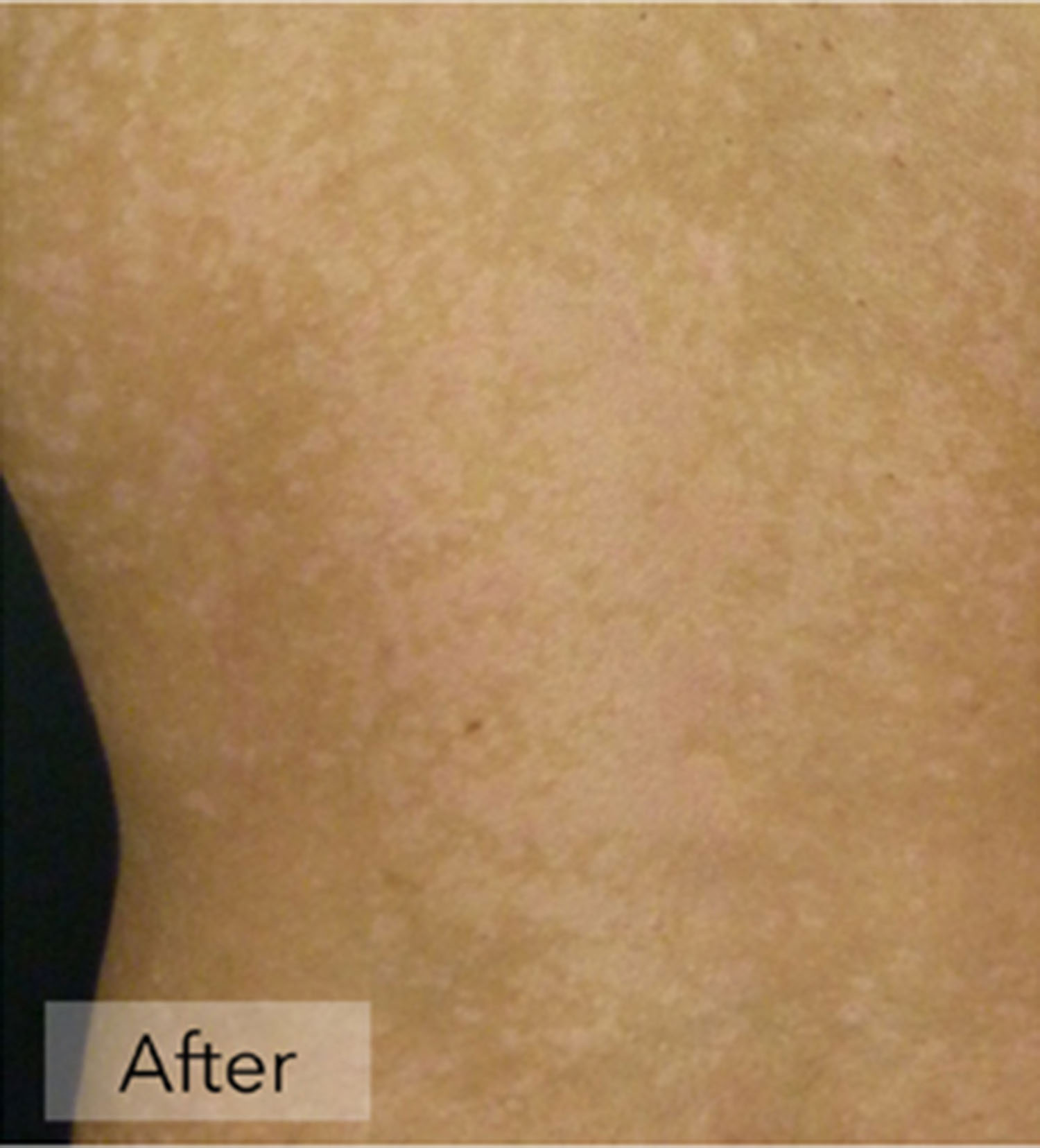
Psoriasis Treatment
The goal is to reduce inflammation and to control shedding of the skin. Moisturizing creams and lotions loosen scales and help control itching. Special diets have not been successful in treating psoriasis, except in isolated cases.
Treatment is based on a patient’s health, age, lifestyle and the severity of the psoriasis. Different types of treatments and several visits may be needed. Dr. Turner may prescribe medications to apply on the skin containing cortisone compounds, synthetic vitamin D analogues, retinoids (vitamin A derivative), tar or anthralin. These may be used in combination with natural sunlight or ultraviolet light. The more severe forms of psoriasis may require oral or injectable medications with or without light treatment.
Sunlight exposure helps the majority of people with psoriasis, but it must be used cautiously. Ultraviolet light therapy may be used, given in a dermatologist’s office, a psoriasis center or a hospital. Photodynamic therapy is a medical treatment that utilizes a photosensitizing molecule (frequently a drug that becomes activated by light exposure) and a light source to activate the applied drug. Although first used in the early 1900s, current photodynamic therapy involves a variety of incubation times for different the light-sensitizing drugs and a variety of light sources depending on the target tissue.
Medical Dermatology
Book an appointment online or call (214) 373-7546 to schedule an appointment to see us in our Dallas or Irving locations.
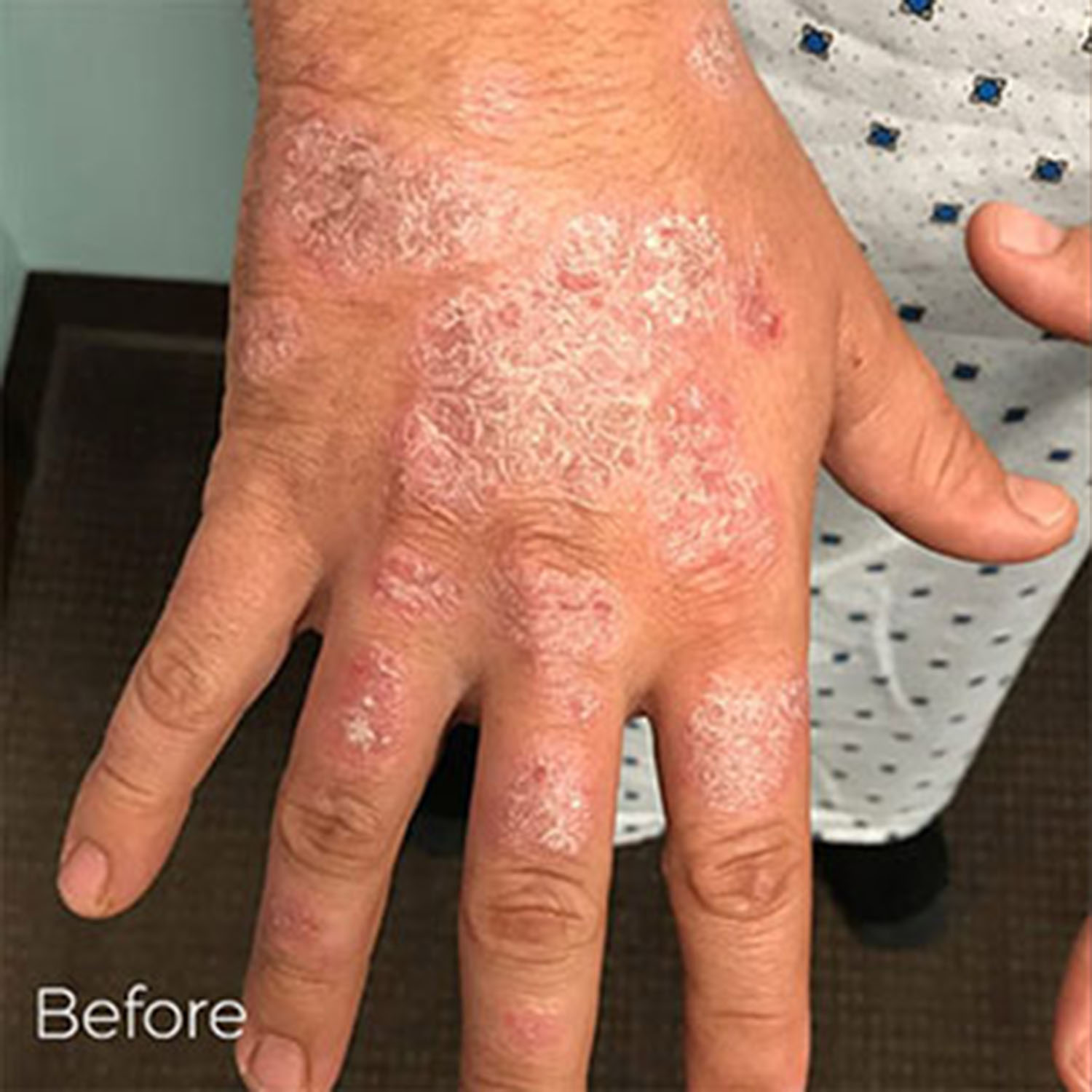
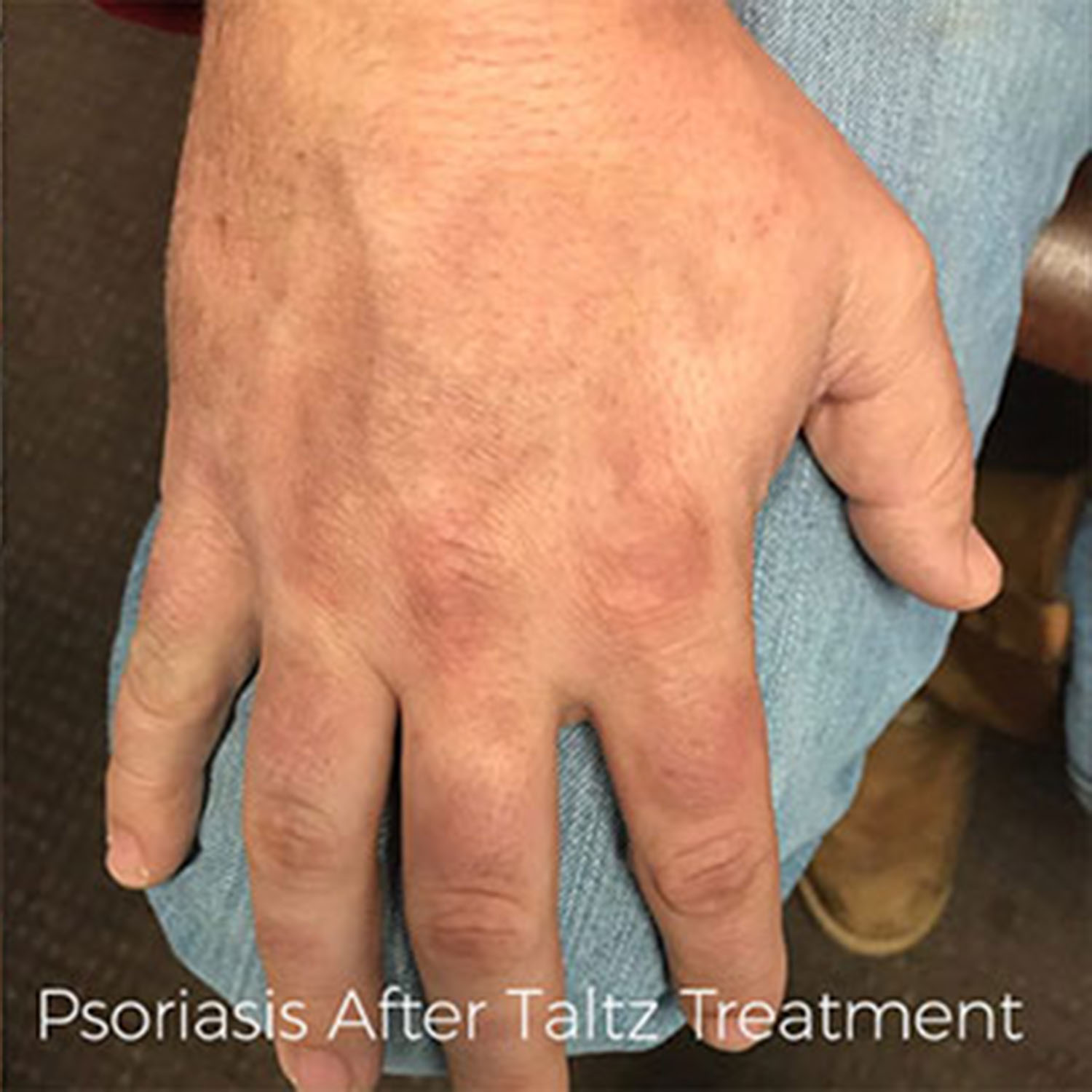
Biologic Agents
The FDA approved the first biologic agent for psoriasis treatment in 2003. Today, dermatologists have a choice of biologics that can be used to treat psoriasis.
A few of the biologics have been approved to treat psoriatic arthritis. Research shows that these biologics may slow or even stop joint damage. This is a significant medical advance. Before the biologics, people with psoriatic arthritis could take medication to alleviate the pain and swelling, but could not prevent joint damage. It may now be possible to prevent the lifelong disability that psoriatic arthritis can cause.
Biologics are given by injection (shot) or infusion (IV). For a few of the biologics, the patient can learn how to inject the medication at home. To receive the other biologics, the patient must go to the dermatologist’s office, psoriasis treatment center or hospital for every treatment.
Patients interested in using a biologic to treat psoriasis should talk with a licensed dermatologist, such as Dr. Ellen Turner. Many people who were not able to control their psoriasis have been helped by a biologic. The biologics also have potential side effects, so it is important to discuss this option. A number of medical tests are required to find out which biologics may be appropriate.
Dr. Turner welcomes such discussions, as she believes in providing outstanding patient care that begins with a conversation to examine specific concerns potential therapies for each patient. A consultation with her will be professional, informative and comfortable. Schedule a visit to discuss the options for treating psoriasis by booking an appointment online or calling the office at (214) 373-7546.
Systemic Medications
Systemic medications are prescription drugs that work throughout the body. They are usually prescribed for patients with moderate to severe psoriasis and psoriatic arthritis. Systemic medications are also used in patients who are not responsive or are unable to take topical medications or UV light therapy. These medications are taken by mouth or given by injection. There are two kinds of systemic medications: traditional systemics, which are created by combining chemicals and have been used for many years, and biologics, a newer class of drugs that are made from human or animal proteins.
Traditional Systemics
Cyclosporine
Cyclosporine is an immunosuppressive drug that stops the activity of certain immune cells, which slows the growth of skin cells. It is taken daily by mouth and should be taken on a consistent schedule. Cyclosporine can provide rapid relief from symptoms. People may see some improvement in symptoms after two weeks of treatment, particularly with larger doses. However, it may take three to four months to reach a complete level of control. It is possible to develop hypertension while on this medication, so blood pressure must be closely monitored. Patients taking cyclosporine should avoid drinking grapefruit juice or eating grapefruit because it can increase the level of the drug in your bloodstream.
Cyclosporine can be used along with the topical drugs. Normally cyclosporine is not used along with UV light therapy. Cyclosporine can increase the skin’s sensitivity to the sun, so protect your skin while in the sun to avoid too much exposure.
Methotrexate
Methotrexate is in a class of medications known as antimetabolites, and was found to be effective in clearing psoriasis in the 1950s and approved for this use by the FDA in the 1970s. Methotrexate binds to and inhibits an enzyme involved in the rapid growth of cells. In people with psoriasis, the drug slows down the rate of skin cell growth. In people with psoriatic arthritis it can reduce painful symptoms. Methotrexate can be used with UVA light therapy to reduce the amount of ultraviolet light needed to clear the skin.
Methotrexate is taken once a week, either by mouth or by injection. It is important to test dose all methotrexate patients prior to starting their therapeutic dose. If it is tolerated, the dosage is increased gradually to achieve clearance. The main risk of long-term methotrexate treatment is liver damage, so patients must be carefully monitored while taking this medication.
Dermatology Office
Meet Dr. Ellen Turner
Dr. Ellen Turner and her staff at the Dermatology Office strive to work within a space where compassion meets technology to obtain top results for Dallas patients.

Soriatane (aciretin)
Soriatane is an oral retinoid, which is a synthetic form of vitamin A. Soriatane was approved by the FDA in the 1980s and is the only oral retinoid approved specifically for treating psoriasis. The exact way that Soriatane works to control psoriasis is unknown. In general, retinoids affect how cells regulate their behavior. Retinoids help control the multiplication of cells, including the speed at which skin cells will grow and shed from the skin’s surface—which speeds up in psoriasis.
Soriatane tends to work slowly for plaque psoriasis. Psoriasis may worsen before clearing begins. It may take up to six months for the drug to reach its peak effect, and it works best in combination with phototherapy.
The most serious risk with Soriatane is the risk of severe birth defects in developing fetuses if a woman has the drug in her body during pregnancy. Soriatane can remain in the body for many months, so it should not be taken for three years before pregnancy.
How much does psoriasis treatment cost?
The cost will vary based on the type and extent of treatment recommended by Dr. Turner.